Insight into schizophrenia disease mechanisms found in the eye
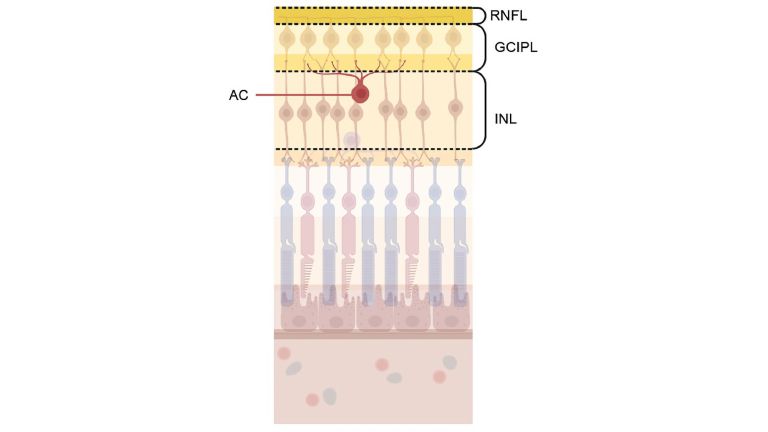
Researchers analyzed the genetic connection of retinal cells and several neuropsychiatric disorders. By combining different datasets, they found that schizophrenia risk genes were associated with specific neurons in the retina. The involved risk genes suggest an impairment of synapse biology, so the ability of neurons to communicate with each other. This impairment might also be present in the brain of schizophrenia patients.
Published: 17.02.2025
The Retina is an outgrowth of the brain and shares the same genetics, making it an easily accessible way for scientists to study brain disorders. In a previous study, the Project Group Translational Deep Phenotyping at the Max Planck Institute (MPI) of Psychiatry, headed by Florian Raabe, found alterations in the retina of schizophrenia patients that became more severe with increased genetic risk. Accordingly, the researchers suspected that Retinal alterations are not only a consequence of common comorbidities like obesity or diabetes, but might be caused by schizophrenia-driven diseases mechanisms directly.
If this is the case, knowing more about these alterations could help researchers understand the biological mechanisms behind the disorder. In addition to schizophrenia, retinal alterations have been observed in patients with bipolar disorder, depression, Multiple sclerosis (MS), Alzheimer’s disease, Parkinson’s disease and stroke. Using data from large studies in the literature, Raabe and first author Emanuel Boudriot (MPI of Psychiatry and LMU Munich) combined genetic risk data from neuropsychiatric disorders with retinal RNA sequencing data. This showed which risk genes were associated with different retinal cells in the above-mentioned disorders.
In two disorders, the data showed a clear connection: First, the genetic risk for MS was associated with retinal immune cells, in keeping with the autoimmune nature of the disorder. Second, risk genes for schizophrenia were associated with a specific class of retinal neurons, the Amacrine cells They are involved in synaptic function, and determine the ability of neurons to communicate with each other. To translate these findings from the cellular to the structural level, the researchers collaborated with Philipp Homan’s working group from the University of Zürich and used results from a UK-based biobank study, which had collected extensive biological data from over 36.000 healthy participants. In this sample, the research team found that the higher the genetic risk for schizophrenia, the thinner the synaptic layer in the amacrine cells was.
Accordingly, both at the cellular and the structural level, Raabe, Boudriot and colleagues showed that neuronal connectivity seems to be impaired in the retina of schizophrenia patients. “Finding this impairment in the Eye suggests that processes in the retina and in the brain are very similar - this would make the retina a great proxy for studying neuronal disorders, because we can examine the retina of patients with a much higher resolution than the brain”, Raabe explains. Understanding the biological mechanisms should help researchers develop more effective and more individualized treatment options.
Retina
The retina is the inner layer of the eye covered with pigment epithelium. The retina is characterized by an inverse (reversed) arrangement: light must first pass through several layers before it hits the photoreceptors (cones and rods). The signals from the photoreceptors are transmitted via the optic nerve to the processing areas of the brain. The reason for the inverse arrangement is the evolutionary development of the retina, which is a protrusion of the brain.
The retina is approximately 0.2 to 0.5 mm thick.
Retinal
A chemical synthesized from vitamin A. Together with opsin, it forms rhodopsin.
Multiple sclerosis
encephalomyelitis disseminata
A common neurological disease that predominantly occurs in young adults. For reasons that are still unclear, the body's own cells attack and destroy the myelin sheaths of nerve cells. This can happen throughout the central nervous system, which is why two different multiple sclerosis patients can suffer from very different symptoms. Common symptoms include visual disturbances, numbness in the arms and legs, but also coordination problems, muscle weakness, and bladder problems.
stroke
Cerebral apoplexy
In a stroke, the brain or parts of it are no longer supplied with sufficient blood, which impairs the supply of oxygen and glucose. The most common cause is a blockage in an artery (ischemic stroke), less commonly a hemorrhage (hemorrhagic stroke). Typical symptoms include sudden visual disturbances, dizziness, paralysis, speech or sensory disturbances. Long-term consequences can include various sensory, motor, and cognitive impairments.
Amacrine cells
Amacrine cells are interneurons of the retina. They are located between photoreceptors and bipolar cells on the one hand and ganglion cells on the other. The name was coined by Ramón y Cajal and means "without axon."
Eye
bulbus oculi
The eye is the sensory organ responsible for perceiving light stimuli – electromagnetic radiation within a specific frequency range. The light visible to humans lies in the range between 380 and 780 nanometers.
Original publication
Boudriot et al., Genetic Analysis of Retinal Cell Types in Neuropsychiatric Disorders, JAMA Psychiatry (2025), doi:10.1001/jamapsychiatry.2024.4230
Retinal
A chemical synthesized from vitamin A. Together with opsin, it forms rhodopsin.