Living with MS

Multiple sclerosis is rightly considered the “disease with a thousand faces.” Every patient has different symptoms and, as a result, different challenges in daily life. But they don’t have to face these challenges entirely on their own.
Scientific support: Prof. Dr. Alexander Flügel, Prof. Dr. Manuel A. Friese, Prof. Dr. Christoph Heesen, Dr. Sina Rosenkranz
Published: 20.02.2026
Difficulty: intermediate
- MS symptoms vary from patient to patient. Consequently, every person affected faces different challenges in daily life.
- Family and friends can help, but so can strangers. They can offer support where MS patients lack the strength or where stairs limit their mobility.
- MS also involves numerous invisible symptoms that are often misunderstood by those around them. As a result, many people with MS are accused of faking their symptoms – an unnecessary, additional burden.
- People with MS can take steps themselves to alleviate certain symptoms and improve their quality of life. This includes, among other things, managing stress effectively, using relaxation techniques, exercising, and following certain dietary practices.
Mind and body influence each other. Studies conducted as early as 40 years ago showed that stress affects the immune system. Glucocorticoids released in response to acute danger reduce the number of certain immune cells in the blood but increase them in the skin. This ensures that immune cells are more abundant where they are needed in the event of injury. However, prolonged, chronic stress weakens the immune system. Conversely, physical ailments also influence mental health. For example, inflammation and brain damage can lead to depressive symptoms. The central nervous system and the immune system communicate with each other via inflammatory mediators and hormones. This communication appears to be disrupted in MS. However, it is unclear whether this was already the case before the onset of MS or is a consequence of the disease.
For Gaby, the visual disturbances have persisted. The 63-year-old with red glasses has had MS for over 30 years. She sees double, which is why she had to give up driving. “I can live with MS,” Gaby says. “But if I had killed a child in a car accident, I don’t know if I could have lived with that.” Because of the MS, she speaks very slowly, but clearly, so it’s easy to follow her. “I owe that to my speech therapist,” says Gaby. Every week she practices difficult words with her.
Multiple sclerosis
encephalomyelitis disseminata
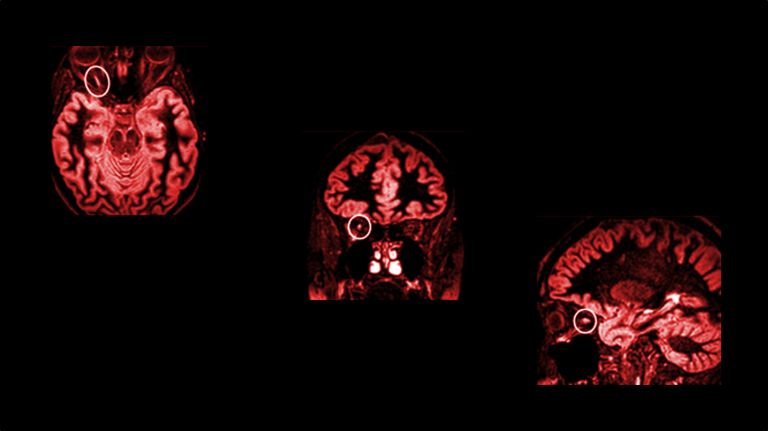
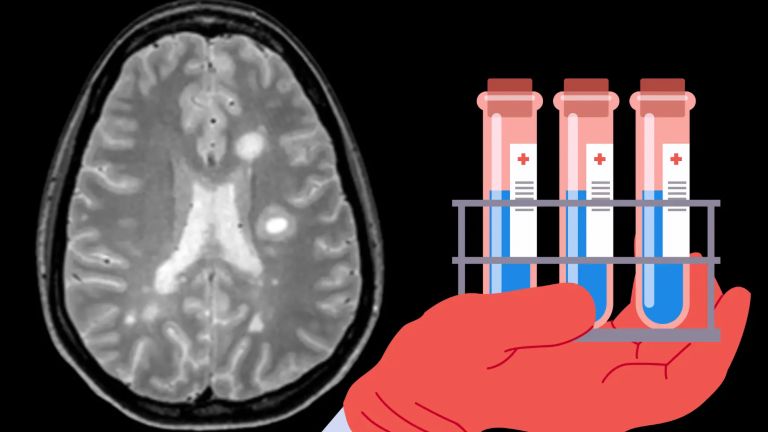
A common neurological disease that predominantly occurs in young adults. For reasons that are still unclear, the body's own cells attack and destroy the myelin sheaths of nerve cells. This can happen throughout the central nervous system, which is why two different multiple sclerosis patients can suffer from very different symptoms. Common symptoms include visual disturbances, numbness in the arms and legs, but also coordination problems, muscle weakness, and bladder problems.
The wheelchair isn’t the end
She has been in a wheelchair for about 10 years now - a fate that is far from inevitable for every MS patient. Gaby’s arms are too weak to properly propel her wheelchair’s wheels, in stark contrast to 53-year-old Bernd: For four years, he’s been zipping through the city in his wheelchair. “I can still walk,” he says, standing up and demonstratively taking a step forward. “But only 20 to 50 meters a day. I have to pace myself carefully.” The wheelchair gives him back some of the mobility that MS has taken from him for nearly 30 years. Without it, he could no longer fully participate in life. With it, he can even cover up to 20 kilometers a day while shopping on his own.
Only stairs remain an obstacle. There, he has to ask other people for help, which not everyone is willing or able to do. After all, not everyone is capable of supporting a man nearly two meters tall like Bernd or knows how to help someone out of a wheelchair. Bernd no longer has any reservations about asking for help.
Barriers in people’s minds
Despite all this, he sometimes gets around on foot as well. “When people see me walking,” Bernd says, “they say, ‘Look, he has a wheelchair, but he can walk!’” Or when he can no longer control his knees and his gait becomes unsteady: “Then some people think I’m drunk.” He has learned to deal with these misjudgments and accusations of faking it from strangers.
But even friends didn’t understand his problems, turned away from him, and called him a “blabbermouth.” Heike – 55 years old and living with MS for 23 years – went through the same thing. She struggles with an invisible MS symptom: fatigue. This is a persistent state of physical and mental exhaustion. “Friends have turned away from me because I couldn’t make it to their party,” Heike says. “They didn’t understand, even though I explained it five times.” This is despite the fact that, for example, fatigue was the most common symptom in the German MS Registry at 58 percent and occurred in 31 percent of patients within the first two years.
Daily life with MS
Fatigue has a huge impact on Heike’s daily life. To cope, she practices “energy management,” as she calls it. She has to plan her day very carefully and can only schedule a maximum of two appointments. On the day of the interview, nothing else was allowed to be on her calendar; otherwise, Heike wouldn’t have been able to manage it. She can do housework, but only in stages. She needs lots of breaks in between, during which she has to lie down. Just sitting isn’t enough. “And when I can’t do anything at all, it just has to wait until the next day,” Heike explains.
Fortunately, her family is understanding: if the groceries aren’t unpacked or the kitchen is a mess after cooking, no one gets angry or annoyed. They know Heike isn’t lazy – she simply lacks the strength to do it. Her family’s understanding and support aren’t just important for Heike. As a study showed, the level of social support available has a strong influence on the quality of life of MS patients.
The role of diet is much discussed. There is not (yet) a scientifically proven MS diet that influences the course or symptoms of the disease. That is why MS patients, like everyone else, are generally recommended to follow a healthy diet rich in vitamins and fiber. There are also numerous guides that recommend certain vitamins and omega-3 fatty acids – though without hard evidence. Heike has found that a low-carb diet helps her with fatigue. “Suddenly I had a little more energy,” she says – even though professional associations don’t yet see enough evidence to make a recommendation. And unfortunately, her diet doesn’t help with Heike’s Memory problems. She has to write everything down so she doesn’t forget it.
Memory
Memory is a generic term for all types of information storage in the organism. In addition to pure retention, this also includes the absorption of information, its organization, and retrieval.
Working with MS
Due to her fatigue, Heike also took early retirement. She was a preschool teacher and, in the end, could no longer manage to tie the shoes of 25 children. Her boss at the time did make her daily work routine easier through various measures. But eventually, even that stopped helping.
Bernd also retired early due to MS and was never able to really get a foothold in his career. Often, he wasn’t even hired in the first place after his potential new boss learned of his condition – a single call to his former employer was enough. Or he was fired during his probationary period after suffering another MS flare-up that sidelined him for an extended period.
Recommended articles
Mental strain
“That made me pretty depressed,” Bernd says. “Because I went from one negative thing to another.” The next flare-up, another job rejection, the separation from his wife at the time, and on top of that, the mental strain of the uncertain course of his MS. Overwhelmed by the situation, he started drinking alcohol. “At some point, I didn’t recognize myself anymore and said: Stop, this can’t go on,” he says. That’s how he ended up in psychological counseling. “It showed me that only I can help myself,” says Bernd.
And that’s exactly what he did. He quit drinking and smoking and started pushing his body again. The former competitive athlete took up jogging once more. As the relapses increasingly limited his ability to walk, he tried to go a little further each day and motivate himself with small successes. “That’s how I tried to regain control over my body,” explains Bernd. Through physical activity, he rebuilt the muscle mass that had been reduced with each MS relapse. Exercise can also alleviate coordination and balance issues and even reduce fatigue. This is because so-called neurotrophic factors are released during exercise, which strengthen the connections between nerve cells and promote the growth of new cells.
Managing Stress
Numerous studies have examined the link between severe stress – such as that caused by stressful life events – and MS. However, this connection appears to be less clear-cut than commonly assumed. “Taken together, studies suggest a small to moderate influence of psychological stressors on disease onset, inflammatory activity, and disease progression in MS,” concluded a summary of 30 studies involving nearly 25,000 patients. In contrast, a clinical study involving 121 patients claimed as early as 2012 that actively managing stress could lead to fewer lesions. However, the supposed lull in disease activity lasted only six months, and the authors had to admit that their anti-stress program offered no clinical benefit.
Gaby, Bernd, and Heike have found their own ways of coping with MS. Above all, they have accepted their fate. None of them can prescribe a formula for dealing with MS. “What helps one person doesn’t help another,” Bernd says as he bids farewell, before racing off in his wheelchair.
Further reading
- von Drathen S et al.: Stress and Multiple sclerosis - Systematic review and meta-analysis of the association with disease onset, relapse risk and disability progression. Brain Behav Immun. 2024 Aug;120:620-62 doi: 10.1016/j.bbi.2024.06.004 (zum Abstract)
- Taylor P, Dorstyn DS, Prior E. Stress management interventions for multiple sclerosis: A meta-analysis of randomized controlled trials. J Health Psychol. 2020;25(2):266-279. doi:10.1177/1359105319860185 (zum Abstract)
- Kern S, Ziemssen T. Brain-immune communication psychoneuroimmunology of multiple sclerosis. Mult Scler. 2008;14(1):6-21 doi:10.1177/1352458507079657 (zum Abstract).
Multiple sclerosis
encephalomyelitis disseminata
A common neurological disease that predominantly occurs in young adults. For reasons that are still unclear, the body's own cells attack and destroy the myelin sheaths of nerve cells. This can happen throughout the central nervous system, which is why two different multiple sclerosis patients can suffer from very different symptoms. Common symptoms include visual disturbances, numbness in the arms and legs, but also coordination problems, muscle weakness, and bladder problems.
Originally published on June 13, 2017
Last updated on February 20, 2026