A Slow Descent into Forgetfulness

Alzheimer’s dementia does not develop overnight. Experts estimate that the disease progresses asymptomatically for about 30 years before symptoms become apparent. Then the fog of forgetfulness thickens in three phases.
Scientific support: Prof. Dr. Frank Jessen, Niklas Behrenbruch
Published: 18.03.2026
Difficulty: intermediate
- Long before an Alzheimer’s diagnosis, the brain is already undergoing deterioration. Experts estimate that the asymptomatic phase of the disease lasts about 30 years.
- Once the accumulation of misfolded Beta-amyloid peptides exceeds a critical threshold, “preclinical Alzheimer’s” begins. The first cognitive deficits become apparent in MCI – MCI stands for “Mild Cognitive Impairment”.
- The actual clinical course of the disease can be divided into three stages in which Dementia continues to progress: from forgetfulness through Memory lapses and personality changes to complete loss of speech and inability to get out of bed.
Beta-amyloid
A peptide consisting of 36 to 42 amino acids that is considered the main component of senile plaques and is believed to be responsible for the development of Alzheimer's disease. The starting product is the amyloid precursor protein (APP). Certain enzymes in the cell membrane cut the precursor protein into peptides of various sizes. Amyloids consisting of 40 and 42 amino acids are found in senile plaques, with the 42-amino-acid product forming aggregates particularly quickly, at least in the Petri dish. The normal function of beta-amyloid has not yet been conclusively clarified.
Dementia
Dementia
Dementia is an acquired deficit of cognitive, social, motor, and emotional abilities. The most well-known form is Alzheimer's disease. "De mentia" means "without mind" in English.
Memory
Memory is a generic term for all types of information storage in the organism. In addition to pure retention, this also includes the absorption of information, its organization, and retrieval.
At some point, Mrs. R. suddenly started acting strangely, a neighbor recalls. One day, for example, she stood at the front door with a stack of bank statements in her hand and tried to open the lock with the bundle of paper. Later, the elderly lady kept showing up at tenants’ doors in the building and insisting on visiting her niece, who had once lived there. Eventually, the spontaneous visits stopped: Mrs. R. was no longer able to climb stairs. She could only leave the apartment with the help of a caregiver and a stair lift – often amid loud cries of protest, as the elderly woman simply no longer knew what was happening to her.
By this point, Ms. R. had likely been suffering from Alzheimer’s Dementia for many years. The disease creeps in slowly. For years, no one notices anything. Then the first seemingly harmless lapses occur: The person affected seems absent-minded and somewhat agitated. Sometimes she can’t find her keys or glasses; other times she gets tangled up mid-sentence and can’t finish it. Then again, she feels unable to read a newspaper article in its entirety or concentrate on the TV news. As the disease progresses, more and more everyday skills are lost. Personal hygiene, eating, getting around – all of these require assistance. The patient becomes dependent on care.
Dementia
Dementia
Dementia is an acquired deficit of cognitive, social, motor, and emotional abilities. The most well-known form is Alzheimer's disease. "De mentia" means "without mind" in English.
Long asymptomatic phase
“Alzheimer’s begins long before the first symptoms become noticeable,” says Wolf D. Oswald, professor of psychology at the University of Erlangen-Nuremberg and head of the Prevention and Dementia Research Group. “As early as after puberty, the first signs of changes leading to Alzheimer’s can be detected, even if the amyloid Plaques only become visible later.” Alois Alzheimer first discovered these deposits – accumulations of misfolded Beta-amyloid peptides – in the intercellular space of the brain of his deceased patient Auguste Deter ▸ Alois Alzheimer – Mad-Doctor with a Microscope. While detection was previously only possible in brain sections from deceased patients, the plaques can now be identified in living individuals using modern imaging techniques, such as Positron emission tomography (PET).
Konrad Beyreuther, one of the world’s leading Alzheimer’s researchers and founding director of the Network for Aging Research at Heidelberg University, estimates the asymptomatic phase to last around 30 years: “Imaging techniques can detect changes in the brain as early as this – and various biomarkers can be detected in the Cerebrospinal fluid 20 years before the onset of the disease,” he says. Experts define biomarkers as characteristic biological features and changes that can, for example, indicate a disease. In the case of Alzheimer’s disease, for instance, elevated levels of beta-amyloid peptides and Tau protein – another altered protein molecule – can be detected.
In line with this, a U.S. research group published a model in 2013 according to which the misfolded beta-amyloid peptides, known as plaques, accumulate slowly over a long period of time. Once a critical threshold – which varies from patient to patient – is crossed, the so-called phase of “Mild Cognitive Impairment” (MCI) begins, which manifests in daily life only through occasional cognitive lapses. For example, those affected have more difficulty retaining new information. Several more years may pass before actual dementia sets in. During this time, a significant decline in brain mass in the Hippocampus can be tracked using magnetic resonance imaging.
Dementia
Dementia
Dementia is an acquired deficit of cognitive, social, motor, and emotional abilities. The most well-known form is Alzheimer's disease. "De mentia" means "without mind" in English.
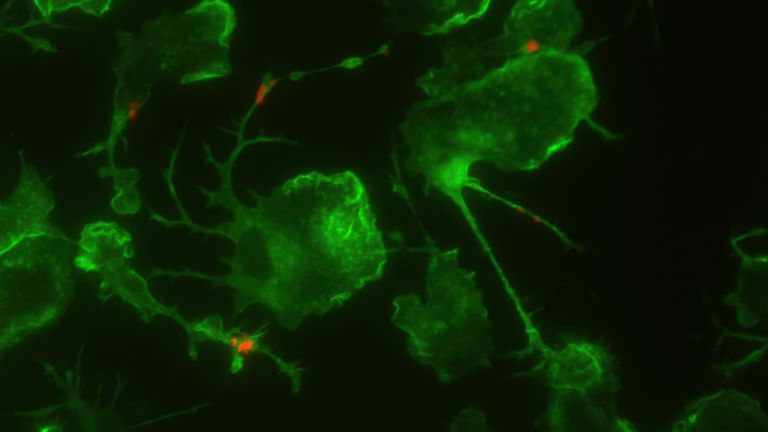
Plaques
Senile plaques
Senile plaques accumulate in the gray matter of the brain when a protein – known as amyloid precursor protein – is not broken down correctly. Inflammation and disorders of fat or sugar metabolism can promote plaque formation. On average, the deposits reach a diameter of 50 micrometers. The appearance of plaques is one of several anatomical changes in the brain that pathologists can use to diagnose Alzheimer's disease after death.
Beta-amyloid
A peptide consisting of 36 to 42 amino acids that is considered the main component of senile plaques and is believed to be responsible for the development of Alzheimer's disease. The starting product is the amyloid precursor protein (APP). Certain enzymes in the cell membrane cut the precursor protein into peptides of various sizes. Amyloids consisting of 40 and 42 amino acids are found in senile plaques, with the 42-amino-acid product forming aggregates particularly quickly, at least in the Petri dish. The normal function of beta-amyloid has not yet been conclusively clarified.
Positron emission tomography
An imaging technique that helps doctors visualize metabolic processes in the body. The patient is injected with a weakly radioactive substance that emits positrons, i.e., beta radiation. When the positrons encounter electrons in the body, energy is released in the form of two photons. These photons travel in opposite directions. Detectors are arranged around the patient in the PET scanner to register the photons that strike them. This makes it possible to track whether the radioactive substance accumulates in certain areas of the body, which can indicate the presence of a tumor, for example. Positron emission tomography is also used in the early diagnosis of dementia. The radiation exposure is low and acceptable in a medical context.
Cerebrospinal fluid
liquor cerebrospinalis
A clear fluid that fills the ventricular system and bathes the brain and spinal cord in the subarachnoid space, protecting them from impact. Three to five times a day, 100 to 160 ml of fluid is renewed by the choroid plexus. Certain diseases are reflected in the composition of the cerebrospinal fluid.
Tau protein
Tau proteins are particularly prevalent in the central nervous system. Their function is to stabilize microtubules – the structures that give cells their shape and support. Under certain circumstances, enzymes attach too many phosphate groups to tau proteins. As a result, the proteins are no longer broken down properly and form toxic aggregates within the neurons. Alongside senile plaques, aggregated tau proteins are considered a classic hallmark of Alzheimer's disease.
Hippocampus
The hippocampus is the largest part of the archicortex and an area in the temporal lobe. It is also an important part of the limbic system. Functionally, it is involved in memory processes, but also in spatial orientation and learning. It comprises the subiculum, the dentate gyrus, and the Ammon's horn with its four fields CA1-CA4.
Changes in the structure of the hippocampus due to stress are associated with chronic pain. The hippocampus also plays an important role in the amplification of pain through anxiety.
Progression in three stages
The early stage is characterized by mild cognitive impairments. Memory declines, those affected forget names and phone numbers and have difficulty concentrating – whether on conversations, texts they’ve read, or the TV news. They often get tongue-tied mid-sentence or search desperately for specific words. Additionally, initial problems with orientation become noticeable, especially in unfamiliar surroundings. For example, finding the way to the restroom in a bar can become a real challenge.
It is not uncommon for those affected to appear depressed during this phase. They react to their changes with grief, fear, and shame. As a result, Alzheimer’s disease in its early stages is often difficult to differentiate from Depression based on symptoms alone. An important distinguishing feature: While people with depression tend to lament their situation, dementia patients tend to cover up their lapses.
It would be better, however, to face up to the forgetfulness. Because if the disease is detected early, there is still room for action. “We cannot cure Alzheimer’s, but we can delay the progression of the disease through appropriate cognitive and psychomotor therapies,” explains Oswald. His observation: When Alzheimer’s patients in the early stages train their perception, coordination, and balance, symptoms can be kept stable over the course of a year. In control subjects without such training sessions, cognitive abilities continued to deteriorate. “The primary goal of such therapy is to improve patients’ quality of life,” says Oswald.
Dementia
Dementia
Dementia is an acquired deficit of cognitive, social, motor, and emotional abilities. The most well-known form is Alzheimer's disease. "De mentia" means "without mind" in English.
Memory
Memory is a generic term for all types of information storage in the organism. In addition to pure retention, this also includes the absorption of information, its organization, and retrieval.
Depression
A mental illness whose main symptoms are sadness and a loss of joy, motivation, and interest. Current classification systems distinguish between different types of depression.
Recommended articles
Forgetfulness on the rise
Language use and comprehension suffer increasingly in the middle stage: Conversations become more difficult, not only due to word-finding difficulties and disordered sentence structure, but because those affected constantly lose their train of thought. They also struggle more and more in everyday life. Skills that were once required daily at work are lost, and driving a car is no longer an option. Times of day and dates get mixed up, and spatial orientation also becomes increasingly difficult – even within one’s own four walls. And while at first only the ability to remember new things seemed to suffer, Long-term memory is now fading as well: memories from the past decades, spouses, children – they all vanish into the fog of forgetfulness. Instead, episodes from childhood and youth sometimes surface – and seem to the person affected as if they had just happened.
Over time, the patient’s personality also changes. Those affected often appear nervous and restless; some feel unloved and suspect that others want to deceive and steal from them. Distrust, irritability, nervousness, and aggressive outbursts – all of these are expressions of the progressive loss of orientation.
Long-term memory
Long-term memory stores information about events, facts, or skills over long periods of time, often for a lifetime. Different types of memory are stored in different areas of the brain. The cellular basis for these learning processes is based, among other things, on improved communication between two cells and is called long-term potentiation.
Physical decline
Toward the end of the middle phase and during the transition to the late stage, daily life for many patients is marked by abrupt mood swings and significant motor restlessness. One moment the patient may have been sitting motionless, and the next they might jump up to march around for hours – within their own four walls. Or, if they are able to leave the house, they may wander aimlessly and without purpose through the streets. Often, people with Alzheimer’s also wander in the middle of the night, as their sense of time is increasingly lost. Day and night, yesterday and tomorrow blur into a single, indistinct mass.
Eventually, even that comes to an end. In the late stages of the disease, the body no longer allows such excursions. Many patients suffer from increased muscle tension and stiff joints. Climbing stairs, personal hygiene, eating – all of this gradually becomes impossible. The patient becomes bedridden and dependent on care.
As the disease progresses, speech also continues to fade. Those affected have only a few words left; many fall completely silent. To communicate with patients, family members and caregivers must now find other ways: Alzheimer’s patients sometimes react with surprising emotion to gentle touch, music, smells, or prayers – especially when these evoke memories from early childhood. With a great deal of empathy, those affected can still be moved even in the midst of the fog of forgetfulness.
Further reading
- Wilson RS, Segawa E, Boyle PA, Anagnos SE, Hizel LP, Bennett DA. The natural history of cognitive decline in Alzheimer's disease Psychol Aging. 2012;27(4):1008-1017. (Zur Webseite).
- Villemagne VL et al; Amyloid β deposition, neurodegeneration, and cognitive decline in sporadic Alzheimer’s disease: a prospective cohort study. Lancet Neurol 2013 Apr;12(4):357 – 67 (zum Abstract).
Alzheimer's disease
Morbus Alzheimer
Alzheimer's disease is a progressive neurodegenerative disorder characterized by cortical atrophy, nerve cell loss, synapse loss, and deposits of amyloid plaques and neurofibrillary tangles, leading to dementia and loss of function. Early symptoms include memory problems, speech disorders, executive deficits, depressive moods, and subtle personality changes. As the disease progresses, global cognitive impairment, aphasia, agnosia, apraxia, and behavioral abnormalities such as apathy, restlessness, and sleep disorders occur. The disease was first described in 1907 by Alois Alzheimer.
Originally published on September 20, 2013
Last updated on March 18, 2026